What are the different Charcot-Marie-Tooth (CMT) types?
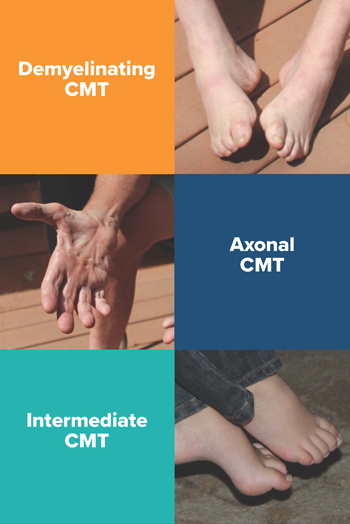
CMT that directly damages the peripheral nerve myelin is known as demyelinating CMT (Types 1, 4 and X). When CMT damages the myelin of the peripheral nerves, the nerve can no longer transmit signals efficiently. This damage causes the speeds at which the nerve transmits its signals to become slowed. Over time, the damage to the myelin causes damage to the nerve axon. Although the axon can become damaged over time, this is still a demyelinating CMT.
CMT that directly damages the peripheral nerve axon is known as axonal CMT (Type 2). When CMT directly damages the peripheral nerve axon, the speed at which the nerve transmits a signal remains near normal, but the overall strength of the signal becomes impaired. This impairment of signal strength can be more severe at the points farthest from the spinal cord (distal) than at points closest to the spinal cord (proximal). Because of this difference, axonal CMT is sometimes known as length dependent axonal CMT.
Intermediate CMT refers to a type of CMT that exhibits peripheral nerve conduction characteristics that overlap that which is characteristic of demyelinating CMT and that which is characteristic of axonal CMT. Intermediate is the name given to this type of CMT because, by nerve conduction characteristics, it is neither demyelinating nor axonal – it is somewhere in between – it is intermediate.
Learn more about how the CMT is accelerating research for Demyelinating and Axonal forms of CMT
What is CMT Type 1?
CMT Type 1 (CMT1) is defined as an autosomal dominant (see inheritance.) demyelinating form of CMT. CMT1 accounts for about 55 percent of all cases of CMT.
Learn more about CMT Type 1 and subtypes
What is Hereditary Neuropathy with Liability to Pressure Palsies (HNPP)?
HNPP is inherited in an autosomal dominant pattern. Like CMT1A, HNPP is caused by changes to the PMP22 gene on Chromosome 17. Unlike CMT1A, where the PMP22 gene is duplicated, one of two PMP22 gene copies is deleted.
What is CMT Type 2
Charcot-Marie-Tooth Type 2 represents axonal forms that are dominantly inherited and make up about one-third of all dominant CMT cases.
Learn more about CMT Type 2 and subtypes
What is Hereditary Sensory Neuropathy?
HSNs typically affect sensory nerves with little to no involvement of the motor nerves. HSNs are an axonal neuropathy and are either autosomal dominant or autosomal recessive in inheritance.
Learn more about Hereditary Sensory Neuropathy
What is SORD?
The newly discovered type is caused by a mutated SORD (sorbitol dehydrogenase) gene that raises sorbitol levels so high they cause nerve damage. Researchers found that treating fruit flies with a diabetes drug (aldose reductase inhibitors) reduced their high levels of sorbitol to near normal.
Scientists at the University of Miami identified 45 individuals from 38 families across multiple ancestries carrying the nonsense c.757delG variant in SORD, in either a homozygous or compound heterozygous state. SORD is an enzyme that converts sorbitol into fructose in the two-step polyol pathway previously implicated in diabetic neuropathy. In patient-derived fibroblasts, there is a complete loss of SORD protein and increased intracellular sorbitol. Furthermore, the serum fasting sorbitol levels in patients were dramatically increased.
Learn more about SORD Deficiency
Find out what is happening in SORD Research
What is CMT Type 3?
Type 3 is a historical term, also known as Dejerine Sottas syndrome (DSS). This was used to describe people with early onset, severe CMT, usually recessive and usually markedly demyelinating (nerve conduction velocities <10 m/s, with normal being >50 m/s in the arms). Both CMT3 and DSS were coined before genetic causes of CMT were identified. Now, with genetic testing, most of these types of CMT are being renamed to a more appropriate term based on the genetics. Some people still use the term DSS as a descriptor, but CMT3 is almost never used.What is CMT Type 4?
All Charcot-Marie-Tooth Type 4 instances of CMT are inherited in an autosomal recessive pattern (see inheritance) and are rare in the United States (~5% of cases). They have various presentations, with some being mild and some severe. These disorders may also have symptoms in other areas of the body, such as cataracts and deafness.
Learn more about CMT Type 4 and subtypes
What is X-linked CMT?
CMTX is a type of Charcot-Marie-Tooth disease that is inherited when there is an affected on the X-chromosome.
What is Roussy-Lévy Syndrome?
Roussy-Lévy does not describe a specific type of CMT, but rather an individual’s symptoms. Roussy- Lévy Syndrome is used to describe a phenotype (or expression of symptoms) that includes high arches, loss of reflexes, distal limb weakness, tremor in the upper limbs, distal sensory loss and gait ataxia (lack of coordination), probably due to the sensory symptoms. This can also be associated with a form of scoliosis called kyphosis. Many people with CMT can have this clustering of symptoms: It really isn’t exclusive to any one type, but the key clinical finding is CMT with a tremor. It doesn’t help define what type of CMT a person has, although it does appear to happen more commonly with demyelinating forms of CMT such as CMT1A and CMT1B. There isn’t a lot of information about Roussy-Lévy Syndrome because it is not a specific disorder and the term isn’t is not really used much anymore (like Dejerine-Sottas Syndrome). To better understand and manage Roussy-Lévy, please consult a CMT expert neurologist and/or genetic counselor.What is Giant Axonal Neuropathy (GAN)?
Giant axonal neuropathy (GAN) is a rare inherited genetic disorder that affects both the central and peripheral nervous systems. The majority of children with GAN will begin to show symptoms of the disease sometime before five years of age. GAN is inherited in an autosomal recessive pattern, which means that both parents of a child with GAN have to carry a copy of the mutated gene. Parents, typically, will show no signs of the disease.
Learn more about Giant Axonal Neuropathy
How many genetic mutations cause CMT?
Since CMT is a multi-gene disorder, there are many different genes that cause the disorder when mutated. Since 1991, more than 100 different genes causing CMT have been identified and the list continues to grow. CMT can be divided into types and subtypes. The types are the clinical pictures of CMT (CMT type 1, 2, 4, X, etc.), usually defined by inheritance pattern and nerve conductions. Subtypes (CMT1A, 2B, 4C, X1, etc.) are given only when the genetic cause is known. Each subtype corresponds to a gene: Every person with CMT2B has a mutation in the RAB7 gene and everyone with CMT4C has two mutations in the SH3TC2 gene.





